The Spike Protein and Autoantibodies to ANXA2: The Driving Force Behind Long COVID?
It was known in 2010 that Spike Protein molecular mimicry may induce ANXA2 autoantibodies.
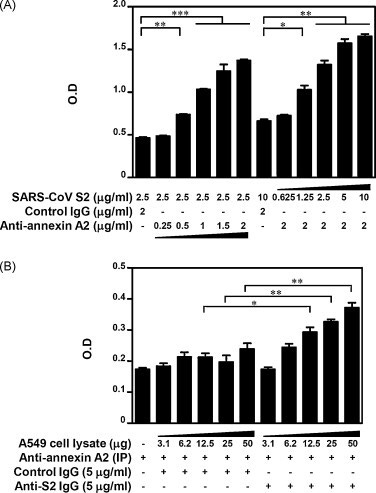
Anti-annexin A2 antibodies bind to SARS-CoV S2 protein and anti-S2 antibodies bind to immunoprecipitated annexin A2. (A) Recombinant S2 protein was coated on ELISA plate with different doses as indicated, then incubated with control IgG or serial doses of anti-annexin A2 antibodies followed by HRP-conjugated anti-rabbit IgG. Cultures were developed using specific substrate ABTS and detected using an ELISA reader. Experiments were carried out in triplicate, and the averages of the relative OD as mean ± standard deviation (SD) are shown. (B) Annexin A2 was immunoprecipitated from various doses of A549 cell lysate using anti-annexin A2 antibodies. Cultures were then incubated with 5 μg/ml of control IgG or anti-S2 followed by HRP-conjugated anti-mouse IgG. Experiments were carried out in triplicate, and the averages of the relative OD as mean ± SD are shown. *p < 0.05; **p < 0.01; ***p < 0.001.
The results you are studying above are not from cutting-edge SARS-CoV-2 research. No. What you are seeing above are the results of a study done in 2010! It was known in 2010 that molecular mimicry of the Spike Protein and ANXA2 was inducing autoantibodies to ANXA2. This may explain a very large part of the pathology of Long COVID.
Readers of my research know that from Day One I have been warning about the (obviously, to me, engineered) molecular mimicry of the Spike Protein and its potential to induce autoimmune disease. This is why I have been so concerned about using the Spike Protein in any therapies. Period.
This was the conclusion reached in 2010:
The local alignment by JEMBOSS-Water analysis showed that the sequence similarity between annexin A2 and two regions on S2 (residues 927–937 and residues 940–951) are 50 and 66.7%, respectively. Our results strongly suggest that SARS-CoV-induced autoimmunity raises an alert not only for effective therapy but also for the development of a safe vaccine.
Annexin A2 on lung epithelial cell surface is recognized by severe acute respiratory syndrome-associated coronavirus spike domain 2 antibodies
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7112629/
Why is this so important, and why would it contribute to the development of Long COVID? Because ANXA2 is essential for breaking down fibrin clots.
ANXA2 is a key player in cell surface fibrinolysis by acting as a co-receptor that orchestrates activation of endogenous tissue plasminogen activator tightly involved in fibrin clearance. Therefore, dysregulation of ANXA2 mechanism may contribute to thrombotic events observed in COVID-19.
And, this is precisely what is happening in those with COVID.
Let us now focus our attention to a paper which was published just last week. This one on SARS-CoV-2:
We determined the kinetics of ANXA2 gene expression in lungs of AC70 hACE2 Tg mice by measuring mRNA levels over the time course of 4 d.p.i. and showed that transcriptional expression of ANXA2 was significantly downregulated between 1-2 d.p.i. The fibrinolytic potential of ANXA2 and its dysregulation have been well documented in vivo and in vitro. ANXA2-null mice (AnxA2-/-) manifested increased fibrin depositions in multiple organs, including lung, heart, and kidney compared to wild type mice, suggesting its importance in maintaining a balanced hemostasis.
The authors of the current SARS-CoV-2 paper claim there is no clarity on the role of autoantibodies in COVID pathogenesis. Yet, isn’t it abundantly clear?
As mentioned above, the exact role of autoantibodies to ANXA2 in the COVID pathogenesis remains unknown and is currently under further investigation. We demonstrated that association between ANXA2 and S100A10 was reduced at 4 d.p.i., the time point when anti-ANXA2 antibodies were presented. Cesarman-Maus et al. [52] raised the hypothesis that anti-ANXA2 autoantibodies may promote hypercoagulation and fibrin deposition by inhibiting t-PA-dependent plasmin formation. This led us to hypothesize that during acute SARS-CoV-2 infection the levels of t-PA may remain sufficient to sustain an effective fibrinolysis, however, the induction of anti-ANXA2 antibodies might negatively affect t-PA binding by disrupting the formation of AIIt complex.
Characterization of Unique Pathological Features of COVID-Associated Coagulopathy: Studies with AC70 hACE2 Transgenic Mice Highly Permissive to SARS-CoV-2 Infection
https://www.biorxiv.org/content/10.1101/2023.10.30.564680v1.full
Again, I cannot even begin to understand why the Spike Protein was used in a gene therapy. Why? And why did the vast majority of doctors and scientists agree it was a “safe and effective” idea?
I will continue my work and seek to find treatments to address this issue. Thank you for reading and thank you for your support.


Doctors are the ultimate herd mentality people. They follow the big pharma and hospital narrative hence choosing livelihood over their oath to protect patient lives. Mercenaries for hire. They stopped actually caring about patients a while ago.
"And, this is precisely what is happening in those with COVID." (Clotting)
Not necessarily! High-dose vitamin D inhibits clots, and in research trials, vitamin C prevented pulmonary clotting in mice expetimentally made septic.
When I had COVID (the original very bad strain), my inflammatory markers elevated considerably, but, being on high-dose Vitamins C and D plus other nutrients, I had NO symptoms of clots, no dyspnea, no SOB, no "brain fog" or other neurological effects, and no reduction of oxygen saturation.
However, I DID experience a considerable drop in energy production and exercise intolerance consistent with mitochondrial impairment/dysfunction that took a long time to learn how to reverse. Mitochondrial damage is a key feature of Long COVID.