BREAKING: Another Mechanism Revealed by Which the Spike (As Amyloid) Can Impair Endothelial Function Inducing “FIP!”
The Presence of Systemic Capillary Leak Syndrome (SCLS): Is This How the Spike Mimics FIP?
From a PrePrint published January 11th:
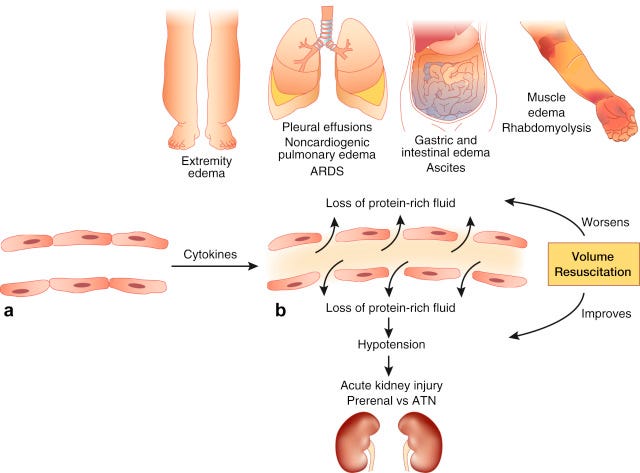
Systemic capillary leak syndrome occurs due to the disruption of endothelial cells, which leads to increased vascular permeability, causing intravascular fluid to leak into the extravascular space and albumin to be retained in the interstitial space.
In general, eliminating the precipitating factor is the cornerstone of SCLS management. SCLS is predominantly managed conservatively in the early stages with osmotic drugs, diuretics, colchicine, renal replacement therapy, hemofiltration, and albumin transfusion. However, in later phases, surgical drainage might be needed to extract the accumulated fluids from body cavities to restore vital organs function.
Capillary Leak Syndrome after SARS-CoV-2 Infection and COVID-19 Vaccines: A Comparative Review
https://www.preprints.org/manuscript/202301.0195/v1
Please note that both SARS-CoV-2 infection and the vaccines can induce this. Therefore, the Spike Protein must be involved.
Now, please understand that this is essentially EXACTLY what happens in the fatal feline disease Feline Infectious Peritonitis!
The inflammation associated with FIP leads to three types of changes in venules. The first is loss of vessel wall integrity, microhemorrhage and leakage of a plasma protein rich in activated clotting and complement activation factors and other inflammatory proteins. A second type of damage involves thrombosis and blockage of blood flow. The third insult occurs in more chronic cases and involves fibrosis (scarring) around the vessels. Variations in these three events determine the amount and makeup of the effusions according to the four Starling’s forces which determine the movement of fluids between the bloodstream and interstitial spaces.
The classical effusion of wet FIP results from mainly from acute damage to the vessel walls and leakage of plasma into the interstitial spaces and eventually into body cavities. Protein leaked into the interstitial spaces attracts more fluids, which can be exacerbated by blockage of venular blood flow and increased capillary pressure. This type of effusion, known as an exudate, also contains high levels of proteins involved in inflammation, immune responses, and blood clotting.
Origin of abdominal or thoracic effusions in cats with wet FIP and reasons for their persistence during treatment
https://ccah.vetmed.ucdavis.edu/sites/g/files/dgvnsk4586/files/inline-files/Persistence-of-abdominal-or-thoracic-effusions-in-cats.pdf
It is now possible to understand how the Spike Protein induces this via it’s amyloidogenic properties.
Whether the monoclonal paraproteins present in SCLS contribute directly to disease pathogenesis is unclear. Purified monoclonal paraprotein from 5 SCLS patients failed to bind cultured endothelial cells or induce any cytotoxicity. Although the amount of monoclonal Ig produced in MGUS is usually small, indicating few clonal plasma cells, it may produce a toxic monoclonal paraprotein that causes pathology either by aggregating and depositing in tissue, such as in light chain amyloidosis, or by binding to autologous common antigens (i.e., acting as an autoantibody) as in cold agglutinin disease, mixed cryoglobulinemia, vonWillebrand syndrome, paraproteinemic neuropathy, and Schnitzler syndrome.
Narrative Review: Clarkson Disease-Systemic Capillary Leak Syndrome
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3017349/
I believe this is certain further evidence of the vast endothelial and amyloidogenic dangers of the Spike Protein.



Wow. My cousin died in May 2021, having spent a month in hospital/skilled care after hysterectomy (new onset cervical/uterine cancer), but had many co-morbidities, including diabetes and kidney failure. After a few weeks at home and then fighting abdominal wound infection, she was back in the hospital with cellulitis, sepsis, and extreme edema where the skin on her thighs was actually weeping large amounts of fluid. Dialysis could not keep up. Another month of hospital & skilled care and finally hospice. There is no doubt that she was multiply jabbed. Would she have died anyway? Possibly, but the downhill slide was quite steep as she was previously living alone and driving herself to shopping, doctors, and dialysis.
It almost seems like an impossible task to get a handle on this f’ing spike. No doubt it was much easier for the FCKs at Chapel-Hill and Ft Detrick ( yes, and Wuhan too) to create the disease than for our seriously underfunded heroes to try to unwind the damage. What the hell is wrong with this picture?